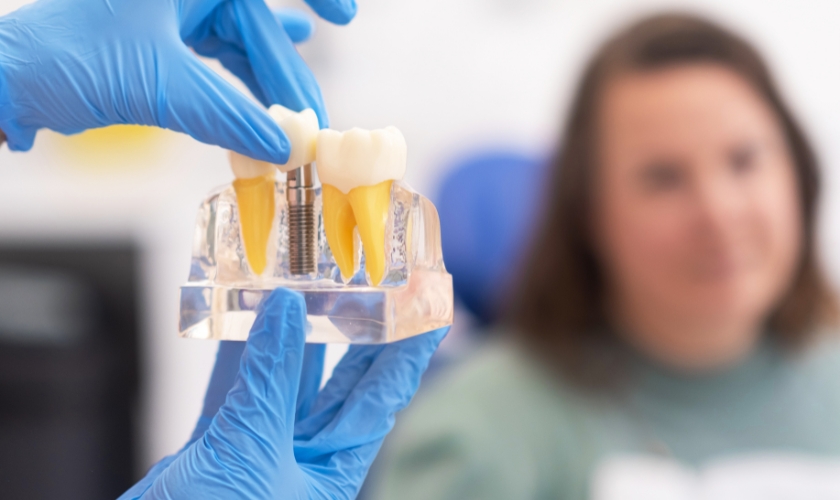
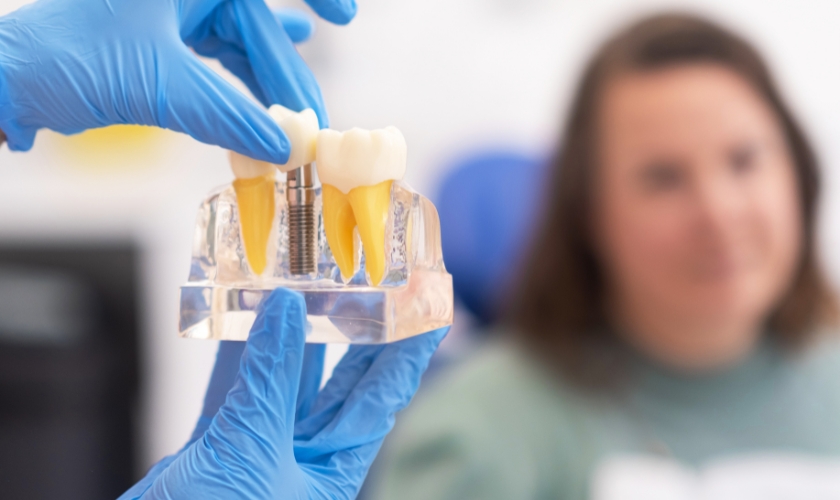
Tooth loss changes more than your appearance. Once a tooth is gone, the ripple effects show up in places you might not expect – the way you chew your food, the way certain words come out, the confidence you feel in a conversation. For many people, these functional changes are far more disruptive than the aesthetic ones.
Dental implants have become the gold standard in tooth replacement precisely because they address these problems at the root. Unlike removable dentures or dental bridges, implants replace the entire tooth structure, from the root to the crown, giving your mouth back the stability it needs to function the way it was designed to.
What Tooth Loss Actually Does to Your Mouth
Most people focus on the visible gap after losing a tooth. What they don’t see is what’s happening underneath. The jawbone beneath a missing tooth begins to deteriorate within the first year because it no longer receives the stimulation it needs from chewing forces. According to research published in the Journal of Dental Research, bone loss at a missing tooth site can reach up to 25% in width during just the first year.
That bone loss doesn’t stay contained — it gradually affects the teeth around it, your bite alignment, and even the shape of your face over time. For residents exploring dental implants, understanding this progression is key to appreciating why timing matters and why implants work so much better than alternatives when placed promptly.
Beyond bone health, missing teeth shift the functional load of chewing onto remaining teeth, create speech patterns your tongue and lips weren’t built for, and can eventually lead to TMJ strain and chronic jaw discomfort. These aren’t minor inconveniences — they compound over time.
How Implants Restore Chewing Function
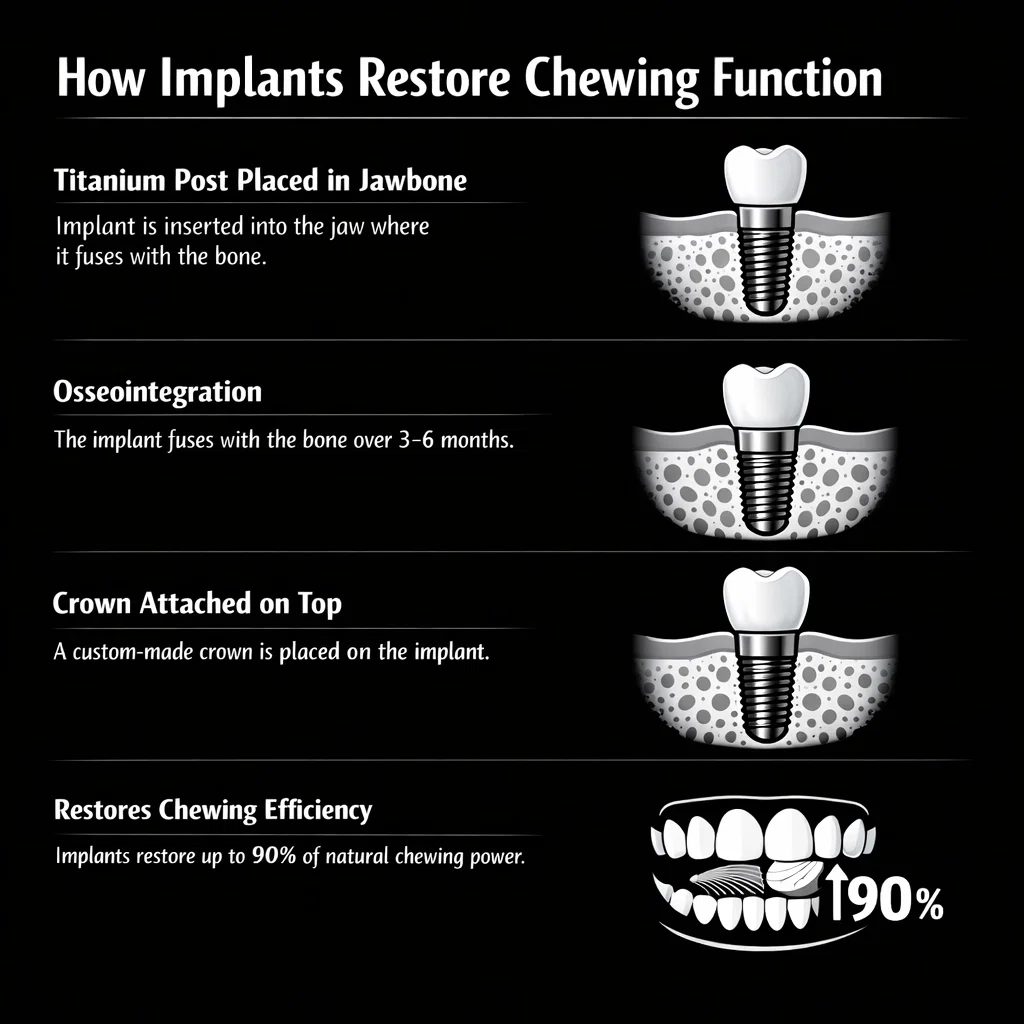
The reason dental implants restore chewing so effectively comes down to how they’re built. A titanium post is placed directly into the jawbone, where it fuses with the surrounding bone through a process called osseointegration. This creates a foundation that mimics a natural tooth root in both structure and function.
Once that fusion is complete (over three to six months), a custom-made crown is attached on top. The result is a tooth that can bear biting and chewing forces comparable to a natural tooth. Studies have shown that implant-supported teeth can restore up to 90% of natural chewing efficiency, compared to conventional dentures, which restore only around 20 to 25%.
Why Dentures Fall Short
Traditional dentures sit on top of the gum and rely on suction, adhesive, or clasps to stay in place. That instability means you’re constantly managing movement when you eat — avoiding certain foods, chewing carefully, or worrying about slippage at the wrong moment. Hard foods, chewy proteins, and even fresh vegetables often end up on the “no” list for long-term denture wearers.
Implants remove that limitation entirely. Because they’re anchored in bone, there’s no movement. You bite down, the implant holds, and your body processes the chewing forces the same way it always did. Patients routinely describe the experience as simply “eating normally again,” which, after months or years of restricted eating, feels like a significant quality of life shift.
The Connection Between Teeth and Speech
Speech is a surprisingly precise mechanical process. Your teeth, tongue, lips, and palate all work together to produce sounds, and when even one piece of that system changes, your speech adapts around it. Missing front teeth affects consonants like “s,” “f,” “v,” and “th.” Ill-fitting dentures can cause lisps, slurring, or clicking sounds that draw attention and create self-consciousness.
Dental implants sit flush in the gum and behave like natural teeth, giving your tongue the correct surfaces to push against. Most patients notice an improvement in speech clarity within weeks of getting their permanent crown. There’s no adjustment period or relearning — your mouth simply has the tools it was missing.
Long-Term Functional Benefits Worth Knowing
The functional advantages of implants aren’t just about the first few months after placement. They’re cumulative. Because implants stimulate the jawbone, they actively prevent the bone resorption that causes the sunken facial appearance common in long-term denture wearers. That means your chewing efficiency and speech clarity are protected for years and even decades down the line.
St. Charles residents have access to implant technology that has been refined significantly over the past two decades. Modern implant placement is more precise, recovery times have shortened, and success rates consistently exceed 95% over ten years, according to data from the American Academy of Implant Dentistry. For most healthy adults, implants are a permanent solution — not a temporary fix.
Who Is a Good Candidate?
Most adults with good general health qualify for dental implants. The key requirements are sufficient jawbone density to support the implant post and healthy gum tissue around the placement site. If bone loss has already occurred, bone grafting can often rebuild the necessary foundation before implant placement – it adds time to the process, but doesn’t disqualify you as a candidate.
Certain conditions, like uncontrolled diabetes, active gum disease, or heavy smoking, can affect healing and implant success rates. A thorough evaluation, including X-rays and a full dental and medical history, will give your dentist a clear picture of whether implants are the right path for you, and what that process would look like.
For those already considering dental implants in St. Charles, a consultation is the best first step – it’s low-stakes, informative, and gives you a realistic picture of what the process involves, what to expect during recovery, and what the outcome will look like for your situation.
Book your implant consultation online today at St. Charles Family Dentistry and take the first step toward eating, speaking, and living without the limitations tooth loss brings.
People Also Ask
Most patients adapt quickly, often within a few weeks of receiving their permanent crown. Unlike dentures, there’s no relearning process because implants function like natural teeth. Your dentist may recommend soft foods during the healing phase after placement, but once the crown is fitted, normal eating is usually restored without a lengthy adjustment period.
Implant failure is rare but possible. The most common causes are infection at the implant site (peri-implantitis), insufficient bone density, poor healing related to smoking or uncontrolled diabetes, and occasionally implant overloading before osseointegration is complete. Choosing an experienced dental team and following post-placement care instructions significantly reduces these risks.
No special maintenance is needed beyond what you’d do for natural teeth — brushing twice daily, flossing, and attending regular dental checkups. The implant itself cannot decay, but the surrounding gum tissue can still develop infection if oral hygiene is neglected. Routine professional cleanings help keep the gum tissue around the implant healthy long-term.
The sooner, the better — but it’s never too late. Getting evaluated promptly after tooth loss helps preserve the jawbone before significant resorption occurs. If too much time has passed, bone grafting may be needed first. Either way, an early consultation with your dentist gives you the most options and the most straightforward path to restoration.